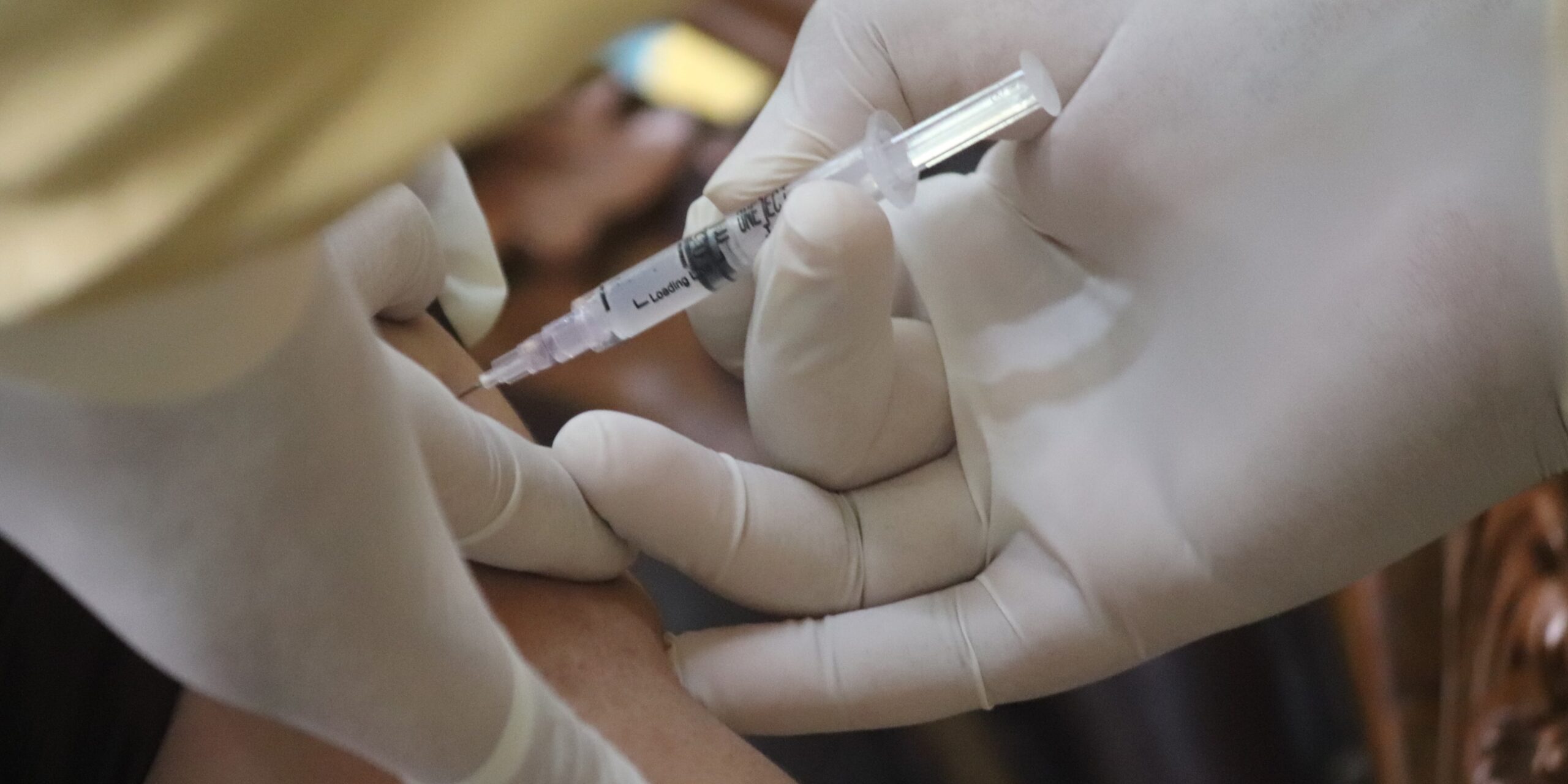
Observing Covid-19 vaccination at the gemba
FEATURE – In his first gemba walk in months, the author observes the Covid-19 vaccination process in a physician’s practice in Wales and reflects on how lean it is.
Words: Dave Brunt, CEO, Lean Enterprise Academy
Photo by Mufid Majnun on Unsplash
I recently visited a local GP practice here in Wales to observe the Covid-19 vaccination process. After so many months spent in isolation, it was wonderful to be at the gemba again. I met fantastic people there and left with many questions, but with enough information to write this account.
The day I visited, the practice – which had just received 400 doses of the Oxford AstraZeneca vaccine – had reserved 100 appointments for their over 80-year-old patients.
Each vial of Oxford-AstraZeneca contains 10 doses (with a possible extra eleventh dose). Once a vial is opened, it must be used within six hours: so long as everyone attended their appointment there would be no wastage. Each patient was scheduled to arrive at two-minute intervals. They would be greeted at the reception desk and asked to go through to one of four clinic rooms. Three of the rooms had a clinician delivering the vaccine and an administrator loading patient information into the computer database. In the fourth room, a clinician carried out both the clinical delivery and the administrative tasks.
ON-SITE PREPARATION
All preparation tasks were “external” to the activity of giving a vaccine. Set-up included discussions on the door-to-door patient flow, stocking up on the items necessary, rearranging furniture in the clinic rooms, and logging onto the IT system in which all appointments had been pre-loaded with patient information. All this needed doing before a patient receives the vaccine. They had planned to start the process at 8.30 AM so they would be ready for the first patient at 9 AM. They were.
The first patient was greeted at reception and asked to walk through the waiting room via a one-way system to the clinic rooms. This was the start of the morning flow. I observed as staff did their job with care, conscientiously and with consideration for others. Lean thinkers have learned from Toyota that work can be documented so that anyone sees whether it is being conducted as designed, making improvement activities more structured. I now needed to visualize what I was seeing, even though the work itself was not the result of proper standardization as we lean people intend it.

Now I could see the work. It involved patients arriving at a desk, being greeted, asked their name and marked as arrived in the booking system. They were invited to sanitize their hands, given a fact sheet and directed into the waiting room. They were then sent through the door and to the next free clinic room. I noted the steps, documented them and timed 10 successive patients, to further understand the current condition. What was happening? Did it happen every time? Did the patients all follow the same steps? Is there a big variance in the time each vaccination takes? I documented what I saw on the Process Study Sheet.

After just over 2 minutes the first patient emerged from a clinic room, vaccinated. They then either waited 15 minutes in the socially distanced waiting room or left immediately.
WHAT REALLY IS THE WORK?
I’d now been observing for 45 minutes but hadn’t seen the value-creating process yet. Observation typically starts at the last process in the system – in this case, the waiting area – and works its way backwards. But here the customer is embedded in the process, which begins at the front door. Because it’s the booking that sets the pace of entry, it was ok to start my observation there.
After booking, I went to observe the detailed steps required to give the vaccine. I sat, socially distanced, in the corner as a lady came into one of the clinic room. She was greeted by the clinician and asked to give her name and date of birth to the administrator who found her on the computer and confirmed her details. This built-in quality check started a sequence of recording information in the database. The clinician then took over, explaining that the vaccine needed to be injected into her arm and asking whether she was left or right-handed and which arm she preferred the injection to be given in. The lady was then directed to sit down, and the clinician explained what the vaccine was, checked there were no contraindications to the patient receiving the vaccine and asked for consent to give it. A syringe and a swab were picked up and an explanation given that the patient would feel very little. The vaccine was injected. The syringe and swab were disposed of and an explanation of how the patient could feel over the next couple of days was given. The administrator then gave the patient a vaccine card, an after-effects leaflet and details of how they would be contacted for their second dose. The patient was asked to re-dress and it was explained that they should not drive for 15 minutes. She was offered a seat in the waiting room. As the patient left the room, the clinician wiped down the chairs and sanitized the area ready for the next patient.
I wrote down the work elements, the discrete steps necessary to complete one cycle. Each element is the smallest increment of work that can be moved to another person. For example, “get syringe and inject patient” is a work element while “get syringe” would not be. It’s important to break work into elements as it helps us identify and eliminate waste (non-value creating activities) buried within the work.
With the work elements defined, the next stage is to time each work element.

The process study shows which of the steps appear to be repeatable with consistently similar times and which have more variation. Work is rarely done the same way every time, but non-repeatable processes cause a huge problem because they make it very difficult to plan and almost impossible to flow.
During the observation it became apparent that some work elements are entirely repeatable, while others more difficult to make repeatable. For example, wiping down after a patient is repeatable, but discussing potential issues post vaccination is more difficult to make repeatable as questions may arise.
Looking at the length of time of the process steps also prompts more questions. The way in which we question whether a process is done by the most effective means can be seen in the image below:

By asking these questions (5W1H), in turn, one can agree whether a step is value creating or not, whether it should be combined with other steps, rearranged or simplified. These are really the four things you can do to improve the safety, quality, delivery or cost of a process. A great example, looking at the Process Study Form is the “undress” step. It’s the longest single time element. Because it was cold on the day I visited, patients had wrapped up well. But three out of ten were very prepared. They had taken their coats off before entering the clinic room and were wearing short sleeves as they had been asked during the booking process (another three also did but undressed in the room) – hence the difference in time.
Whilst time and purpose resulted in us not reconstructing the Process Study Form to eliminate, combine, rearrange or simplify the steps, that is really the point of looking at work in such detail. The correct way to do this is to give front-line workers the skill to look at their work so they will be able to come up with much more appropriate countermeasures than any centralized staff, improvement expert or outsider ever could.
CAPACITY AND PULL
I was interested in the capacity of the system. To understand this, I did a rough calculation of the “lowest repeatable time” of each work element (not the fastest time, but the time a team member could safely repeat the work). I worked out that the lowest repeatable time to administer a vaccine is 2 minutes and 45 seconds in its current guise.
Patients are booked to arrive at two-minute intervals. If nothing were improved, but this time used to plan how many clinics are required, then two clinics staffed by a vaccinator and administrator (rather than 4) would be needed. The calculation here is Total work Content/Takt = No of people (in this case clinics, each operated by two people.) The point here is that anyone can throw people at a problem, but understanding the total system is what’s necessary to optimize flow.
Moving forward there will be two separate activities. First dose and second dose. Many of the activities required for the first dose will not be needed. What will be the work? How will it be designed? How many clinics will be needed? Using these analytical tools, the answers to these questions become much easier to develop.
THE NEED FOR A LEANER SUPPLY
Arguably, our biggest problem is not the vaccination process, but getting supplies. In Wales, GPs haven’t been given either firm delivery dates or quantities of vaccines they will receive. This means they can only plan clinics once they have received the vaccine, which increases lead-time. However, knowing the cycle time is key to design the supply chain. By understanding the work, it is possible to calculate the number of clinics required, overlay how many centers are needed and then design the delivery system.
If Covid-19 vaccinations are to be a part of every-day life we aren’t going to be able to rely on the good-will of volunteers nor are we going to be able to add such an endeavor to the ever-growing list of activities that we require healthcare professionals to do. Resources are already stretched, so thinking through the work to be done and the design of the supply chain will be critical moving forward.
Outside of Covid-19 vaccines, NHS supplies currently make weekly deliveries to surgeries in Wales – a very unresponsive system. To provide exactly what the customer wants, when they want it, in the quantities wanted, organizations must compress the order-to-delivery lead-time and deliver small quantities regularly, just in time. This removes peaks and troughs from the supply chain, reduces the amount of stock required to be stored and dramatically increases the velocity of product delivery. A good summary of the benefits vs myths of JIT are available here.
To implement this cost effectively, healthcare supply providers need to map the extended value stream. This needs to be done now to avoid supply issues in the process moving forward. Without such exercises, the opportunity to develop insights will be missed. I am sure that the front line will deliver, but will have done so with much overburden. We will get through this current crisis but will not have questioned the underlying thinking of how we are organized to mass vaccinate.
We must get ahead of the issues we’ve encountered during the pandemic. The problem to solve is how to increase the velocity of the total process and vaccinate as soon as possible to save lives, then to set up processes to be able to do this safely, in the shortest possible time in the future.
A longer, earlier version of this article first appeared on the Lean Enterprise Academy blog, the second part of an article on applying Lean Thinking to the vaccination process.
THE AUTHOR

Read more


FEATURE – The author explores the relationship between kanban and improvement and discusses how using it can impact our lean transformation.


FEATURE – The many benefits of 5S are well known, but few people realize the positive impact the technique can have on our environmental performance, says our lean and green correspondent after visiting Tokheim Italia.


COLUMN – Want to grasp the current situation? Then you must go to the gemba, but it would be a mistake to think that alone is enough to change your business… you also have to ask why and show respect.



ARTICLE - To operate successfully we need systems, but as we grow these often give us "big company disease." The solution is bringing leadership at work level to really guarantee customer satisfaction.

